Editor’s Note: This post was updated on July 20, 2018, for accuracy and comprehensiveness. It was originally published on July 1, 2015.
by InBody USA
The term “skinny fat” has been around for a while now, but it seems to have started trending following a feature in TIME Magazine. In it, outwardly skinny and visually healthy people were surprised to learn that they had the same medical issues as an obese person.
Bottom line, looking skinny doesn’t mean you’re healthy if you are skinny fat.
If you’re a little unclear on what exactly skinny fat means, it refers to someone who has a weight and BMI that is normal for that person’s height but has much more fat than and not enough muscle recommended for optimal health.
Many people just assume that if their weight and/or BMI is normal, they have nothing to worry about. This has a lot to do with misconceptions about BMI’s usefulness in assessing weight and health. For example, according to the World Health Organization (WHO), if your BMI is between 18.5 and 24.99, you are considered to be in the normal range for sufficient health. So if you have a BMI of 22, you’re automatically in the clear, right?
Not so fast – although the WHO has set these ranges, they are quick to qualify them with the following:
[BMI] should be considered as a rough guide because it may not correspond to the same body fat percentage in different individuals.
Source: WHO
The fixation on weight, thinness, and BMI is where so many people get fooled into living unhealthy lifestyles. They feel like exercising daily and eating a healthy diet doesn’t apply to them because they look skinny. But looking the part doesn’t always mean you fit the part.
As Long as I Look Good, That’s All That Matters!

If only that were the case.
Unfortunately, that attitude is exactly what causes people to become skinny fat in the first place. The appearance of being skinny seems to outweigh being fit and healthy. However, because of the way fat can be stored, skinny fat people risk having serious health problems.
Not all fat gets stored under the skin. Fat that people can see is referred to as subcutaneous fat, but there’s a second type – visceral fat – and it’s the worse of the two. If you’re skinny fat, you likely have a lot of this second type.
Visceral fat is internal fat that develops in the abdominal cavity, gets stored around the organs, and wraps around your kidneys, intestines, stomach, and liver. It’s sneaky because while it’s easy to see subcutaneous fat, it isn’t so easy to see the visceral fat in your midsection.
Having large amounts of visceral fat can spell a heap of trouble, according to Harvard Medical School. Visceral fat has been linked with:
So while on the exterior, skinny fat people might look attractive, on the inside, their bodies may be at high risk for a number of health problems and syndromes.
How can you tell if you’re skinny fat? It’s not as easy as looking in the mirror or standing on a scale. You need to understand what your weight is made of.
It’s Not Just About Weight

How your weight is distributed determines whether you fall into the skinny fat category. Weight alone cannot tell whether you’re skinny fat or not, which is precisely why so many people don’t realize that they are.
The term “skinny fat” is actually a popular term that describes a very real medical condition called sarcopenic obesity. This condition refers to an individual who may have what would be considered a normal/healthy weight, but metabolically, this person shares many health characteristics as someone who is overweight or obese
A person who is sarcopenic obese will have high fat mass and low muscle mass.
One of the best ways to determine whether you may be skinny fat is to have your body composition analyzed and your percentage of body fat determined.
How to Tell If You’re Skinny Fat
Once you’re able to get reliable information about your body fat percentage, you can compare it against the recommended percent body fat ranges. The recommended ranges for healthy men are between 10-20% body fat, and for women, the ranges are 18-28%.1
If your body fat exceeds these ranges, but you have a normal weight when you stand on the scale, you may be skinny fat.
There are several ways to have your body composition analyzed, all of which come with differing degrees of convenience and accuracy. Here are three ways to measure body composition:
Calipers
Probably one of the most common forms of body composition analysis. Calipers operate by pinching the fat that is held just under the skin (subcutaneous fat) and estimating the internal (or visceral) fat, which is where many skinny fat people hide their weight.
Getting consistent results from test to test can be an issue as well because each test administrator will have a different degree of skill than the person who conducted the test before. Even if it is the same person conducting the test, there is always the risk of human error (pinching softer/harder, etc.) with each test.
So, although this is probably the most accessible way to measure your body fat, it won’t be the most accurate. This is because calipers only actually measure the subcutaneous fat and then use prediction equations or tables based upon your age to guess the visceral fat.
Clinical Tests
It is possible to have your body composition determined in a clinical setting using tests and procedures such as hydrostatic weighing and dual x-ray absorptiometry (DEXA). However, these procedures both require specialized equipment, and in the case of DEXA, exposes your body to low levels of radiation. Although both of these tests are regarded as being highly accurate, because of the limited access, they may not be the easiest to access for regular testing to track changes in body composition.
BIA Scales and Devices
BIA devices are devices that use small electric currents to measure body composition. These are the body composition results of someone who fits the skinny fat/sarcopenic obese body profile:
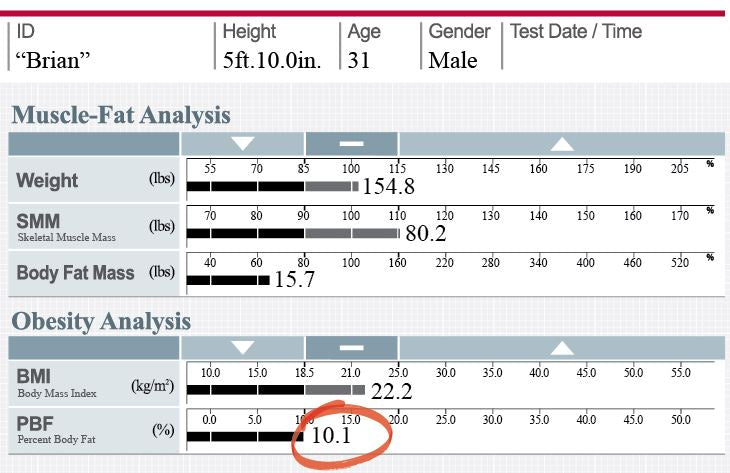
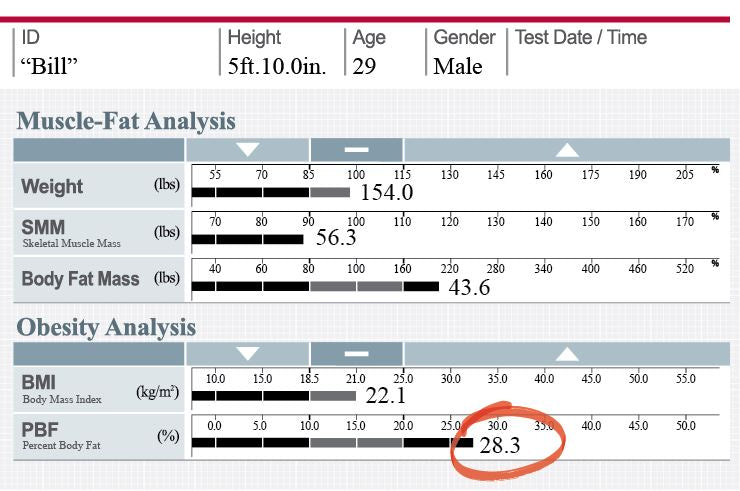
Below are results from an InBody Test, a medical body composition analyzer:

This section is taken from the InBody Result Sheet.
For this person, who is a 5’4” female, 135.3 pounds is just above her ideal weight, but within what is considered normal (BMI 23.2). However, it’s clear to see that this person does not have enough Skeletal Muscle Mass and has excessive body fat. If you do the math, this person has a body fat percentage of 35.0%. This surpasses all upper limits of percent body fat ranges, which are usually around 28%.
BIA devices are quick, easy to use, and depending on the manufacturer, can be quite accurate in determining body composition results for all areas of the body – including the abdominal area, where visceral fat builds up over time.

Visceral Fat area over 100 square meters increases the risk for metabolic syndrome.
When using a BIA device, it’s important to look into how the device you are using determines body composition and how accurate its results are. Some handheld devices may only directly measure your arms and estimate the remainder, while others may only directly measure your legs and estimate the upper body. Whenever possible, use a BIA device that directly measures the entire body for the most accurate results.
If you find out you are skinny fat through body composition, the next step is to figure out how to improve.
How Do People Become Skinny Fat?

First, you need to understand how you may have become skinny fat.
Essentially, the net result of losing muscle mass (and decreasing metabolic rate) and gaining fat mass due to maintaining the same caloric intake with a lower metabolic rate creates the skinny fat condition. Diet and exercise (or lack thereof) play key roles here.
Carbohydrates and foods that are high in calories are great for creating energy potential in the body, but if that energy is not used through activity and exercise, it will become stored in the body as fat.
Similarly, muscle mass decreases over time when the muscles are not being used. If you work in a 9-5 job that requires you to be seated and not move around for most of the day, skeletal muscle mass is likely to decrease over time. Fat mass will also increase as mobility decreases.
Sitting all day, eating an unhealthy diet, and skipping workouts is a recipe for muscle loss and fat gain. Many people have sedentary lifestyles due to work and are prime candidates for muscle loss and fat gain if they don’t do anything to guard against it.
However, this isn’t the only way muscle loss and fat gain can occur.
Michael Matthews over at Muscle For Life, in an exceptionally well-researched piece, has another take on how people become skinny fat. Instead of losing muscle because they don’t exercise, he shows that people can lose muscle because they don’t diet and exercise the right way:
Conventional weight loss advice:
- Severe calorie restriction
- Excessive amounts of cardio
- Minimal weightlifting with an emphasis on high-rep training
If you try to cut calories, while at the same time run on a treadmill an 1 hour a day 5 days a week, your body may not have the energy it needs to perform. After a certain point, your body will start metabolizing muscle because it needs energy once the other options are exhausted. Weight loss will occur at the expense of both fat and muscle loss, which will do very little to improve body fat percentage and becoming less skinny fat.
Now that you understand the cause, here is the solution.
How To Overcome Being Skinny Fat
 It all goes back to improving your body composition.
It all goes back to improving your body composition.
People who want to be thin and healthy need to increase their muscle mass and reduce their fat mass.
This can be done in a number of ways, such as eating a protein-rich diet, but one of the best ways is to increase Skeletal Muscle Mass from weight training that focuses on heavy, compound exercises.
Why weight training? Lifting heavy weights is the best way to increase muscle growth, and correspondingly, Lean Body Mass.
With increased lean body mass, your Basal Metabolic Rate (BMR) increases. In plain speech, the higher your BMR, the more calories your body naturally burns when it is doing nothing (i.e. sleeping). The more calories you burn at rest, the greater the fat loss.
If you are worried that building muscle might make you look bulky instead of skinny, don’t! Muscle is much denser than fat, meaning that if you weighed the same as you do now, but you had more muscle than fat, you would actually appear thinner. Except in this thin body, you would be healthier.
Most people don’t know that muscle is also heavier than fat. So, perhaps ironically, if you were to increase your muscle/Lean Body Mass to the point where you were able to reduce your body fat percentage significantly, you may actually weigh more than you did when you had a skinny fat body.
This is why understanding your body composition is so important. If you were just measuring your weight with a scale and judging your appearance in the mirror, you may have never known you were potentially at risk for health problems.
Also, misunderstandings about building muscle/gaining weight due to muscle may have led you to avoid strength training altogether and instead focused on insane levels of cardio coupled with calorie restriction. This is how many people become skinny fat in the first place.
So, now you know the facts. Just because someone looks skinny, don’t just assume they are healthy. Don’t aspire to be skinny, aspire to be healthy. Because at the end of the day, being healthy is always attractive.





 When most people think about
When most people think about  Many are already aware of the connection between
Many are already aware of the connection between